Endometriosis is a painful condition. It happens when tissue similar to the uterine lining grows outside the uterus. This tissue responds to hormonal changes just like normal uterine tissue does. It thickens, breaks down, and bleeds but has nowhere to go. Over time, this causes inflammation, scarring, and intense pelvic pain. There are four stages of endometriosis, from minimal to severe. Endometriosis Stage 4 is the most serious.
Stage 4 endometriosis involves deep implants, large ovarian cysts, and widespread scar tissue. It can affect the ovaries, bowel, bladder, and fallopian tubes. Many women with this stage experience severe pain and fertility challenges. It doesn’t affect life expectancy, but it can seriously impact your daily life. The good news? With the right diagnosis and treatment, symptoms can be managed effectively.
Related Post: Which Size of Fibroid is Dangerous
Table of Contents
ToggleEndometriosis Stage 4
Endometriosis is a condition where tissue similar to the uterine lining grows outside the uterus. It affects millions of women worldwide, and understanding each stage is critical for getting the right care. Stage 4 endometriosis — also called severe endometriosis — is the most advanced form of the disease, and it can significantly impact your quality of life if left untreated.
There are four stages of endometriosis: Stage 1 (Minimal), Stage 2 (Mild), Stage 3 (Moderate), and Stage 4 (Severe). The difference between stage 3 and stage 4 endometriosis is the extent of the tissue growth. Stage 4 is characterized by widespread deep implants, large ovarian cysts called endometriomas, and extensive pelvic adhesions or scar tissue in the pelvis. These deeply infiltrating lesions often involve the ovaries, fallopian tubes, bowel, and bladder — making it the most complex stage to diagnose and treat.
So, how serious is stage 4 endometriosis? While stage 4 endometriosis doesn’t typically affect life expectancy, it can cause debilitating pain and serious complications, including infertility. Early diagnosis through imaging and laparoscopy, combined with a personalized treatment plan, can make a real difference in managing the condition effectively.
Stage 4 Endometriosis Symptoms
Recognizing the symptoms of advanced endometriosis early can help you seek timely care. The signs of this condition can vary, but they often become more intense as the disease progresses. Here’s what to watch out for.
Many women live with these symptoms for years before receiving a proper diagnosis. That’s why knowing what stage 4 endometriosis symptoms look like is so important — it empowers you to advocate for yourself when speaking with your doctor.
Severe Pelvic Pain
Severe pelvic pain is the hallmark symptom of stage 4 endometriosis. This isn’t just ordinary menstrual discomfort — it’s often described as sharp, stabbing, or throbbing pain that can make daily tasks nearly impossible. The pain typically worsens during menstruation and can persist throughout the month due to chronic pelvic pain caused by deep infiltrating endometriosis.
Painful Bowel Movements
When endometrial tissue grows near or on the rectum, it can cause significant pain during bowel movements. Many women also experience bloating, constipation, or diarrhea — especially around their periods. Pain during bowel movement is one of the most telling signs of advanced endometriosis and shouldn’t be ignored.
Painful Intercourse
Painful intercourse — or dyspareunia — is a common and distressing symptom. The pain often occurs during deep penetration and can linger for hours after. This symptom is frequently linked to endometriosis adhesions and deep implants affecting the vagina, uterosacral ligaments, or nearby structures. It’s one of the key painful intercourse causes associated with endometriosis.
Irregular Periods
Heavy menstrual bleeding, known as menorrhagia, is another red flag. Women with stage 4 endometriosis may also notice spotting or bleeding between cycles. These irregular periods occur because the endometrial tissue responds to hormonal fluctuations, just like the uterine lining does — but it has nowhere to go.
Pain When Urinating
When endometriosis spreads to the bladder or urinary tract, it can cause sharp pain or burning during urination. This symptom often gets misdiagnosed as a urinary tract infection. If you’re experiencing recurring bladder discomfort without infection, endometriosis could be the underlying cause — particularly at the severe stage.
Infertility
Endometriosis and infertility are closely linked, especially at stage 4. The disease can block or damage the fallopian tubes, impair ovarian function, and create a hostile environment for egg fertilization. If you’re having trouble conceiving, endometriosis diagnosis should be part of the conversation with your gynecologist. Fortunately, there are options — including assisted reproductive techniques like IVF — that can help.
Other Symptoms
Beyond the physical symptoms, many women experience fatigue, low mood, and anxiety as a result of living with chronic pain. These emotional and mental health impacts are just as real as the physical ones and deserve attention as part of a comprehensive endometriosis management plan.
Stage 4 Endometriosis Treatment
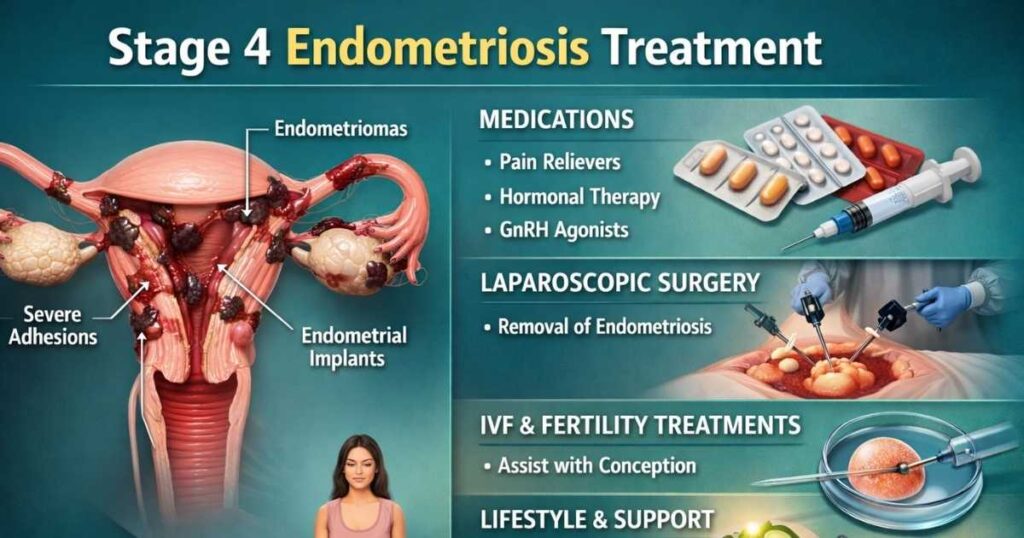
It’s important to understand upfront: there’s no permanent cure for endometriosis at any stage. However, there are several effective treatment for severe endometriosis options that can control symptoms, preserve fertility, and significantly improve your day-to-day life. The best treatment for advanced endometriosis depends on multiple factors, including your desire for pregnancy, the severity of your symptoms, and the location of the endometrial implants.
Your doctor will work with you to create a personalized treatment plan. This might include medications, hormonal therapy, or surgery — or a combination of all three. Let’s break down each option.
Medications
For many women, the first line of defense against endometriosis pain is over-the-counter pain relief. Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can help manage menstrual cramps and pelvic pain. While these don’t treat the underlying condition, they can provide meaningful relief for day-to-day symptoms. Your doctor may also prescribe stronger pain medications if over-the-counter options aren’t enough.
Hormonal Therapies
Hormonal therapy for endometriosis works by suppressing the menstrual cycle and reducing estrogen levels, which slows the growth of endometrial tissue. Several options are available. Combined estrogen-progesterone contraceptives — available as pills, patches, vaginal rings, injections, or IUDs — are often prescribed to reduce heavy menstrual bleeding. Progestin-only options can suppress menstruation entirely. Gonadotropin-releasing hormone (GnRH) antagonists and agonists are more advanced medications that stop the ovaries from producing estrogen and progesterone, effectively creating a temporary menopause-like state to control endometrial growth.
It’s essential to note that hormonal treatments are generally not recommended for women who are actively trying to conceive. If pregnancy is part of your plans, have an open and honest conversation with your specialist before starting any hormonal therapy for endometriosis.
Surgical Options
Surgery is often recommended for stage 4 endometriosis, particularly when symptoms are severe or fertility preservation is a priority. The goal of surgery is to remove or destroy endometrial implants, endometriomas, and adhesions. There are three main surgical approaches, each suited to different clinical situations.
1. Laparoscopy
Laparoscopic surgery for endometriosis is the most commonly used and least invasive surgical option. The surgeon makes small incisions in the abdomen and inserts a thin, lighted tube with a camera — called a laparoscope — to directly visualize and treat the affected areas. Using tiny instruments and tools like lasers or scalpels, the surgeon removes or destroys the endometrial tissue, cysts, and scar tissue. This procedure also allows for simultaneous diagnosis and treatment. For stage 4 cases with deep infiltrating endometriosis, the surgeon may use both excision (removal) and ablation (destruction) depending on the location and depth of the implants.
2. Hysterectomy
A hysterectomy — the surgical removal of the uterus — is sometimes recommended for women with severe, treatment-resistant pain who don’t wish to become pregnant. In some cases, the ovaries may also be removed (oophorectomy) to reduce estrogen production and limit recurrent endometriosis. While hysterectomy for endometriosis can provide lasting pain relief, it’s a major decision with permanent consequences. If you’re considering this option, discuss it thoroughly with your doctor — and if you still wish to have children, ask about egg freezing and surrogacy before proceeding.
3. Laparotomy
Laparotomy is an open abdominal surgery used when laparoscopy isn’t feasible — typically in very complex or severe cases where deep implants are located in hard-to-reach areas. Through a larger abdominal incision, the surgeon gains direct access to remove endometrial tissue, cysts, and adhesions. It’s performed under general anesthesia and requires a longer recovery time than laparoscopy. While it’s not the first choice, laparotomy remains an important surgical option for the most challenging endometriosis complications.
Summary
Living with stage 4 endometriosis is challenging, but it doesn’t have to define your life. Alongside medical treatments, certain lifestyle strategies can help you cope more effectively. Pelvic floor exercises can strengthen the pelvic muscles and reduce discomfort. A balanced, anti-inflammatory diet — and reducing caffeine and alcohol — may help manage symptoms. Stress management through yoga, meditation, or mindfulness can also play a supportive role. Complementary therapies such as acupuncture, herbal therapy, chiropractic care, massage, and Ayurveda have shown promise for some women as well.
Before trying any of these approaches, it’s important to get a proper endometriosis diagnosis so you understand the size, location, and stage of your condition. Always consult a qualified specialist before starting any new treatment or lifestyle protocol.
Conclusion
Stage 4 endometriosis is serious, but with the right care and support, you can manage it effectively. Whether you’re navigating chronic pelvic pain, exploring endometriosis treatment options, or trying to understand how it affects your fertility — you don’t have to face it alone. Early diagnosis, a specialist-led treatment plan, and a proactive approach to your wellbeing can make a significant difference in your quality of life. If you’re experiencing any of the symptoms discussed in this guide, please speak with a healthcare provider as soon as possible. The sooner you get answers, the sooner you can begin your path to relief.
If you still have concerns or need expert guidance, the team at Aval Clinics is here to help. Reach out today for personalized care and a consultation tailored to your needs.
FAQs
Can stage 4 endometriosis be cured?
There’s no permanent cure for endometriosis at any stage. However, surgery and hormonal therapy can effectively manage symptoms and improve quality of life for most women.
Does endometriosis cause cancer?
Endometriosis is not cancer, but women with severe endometriosis may have a slightly elevated risk of certain ovarian cancers, particularly endometrioid and clear cell carcinoma. Regular monitoring is advised.
Can endometriosis come back after surgery?
Yes, recurrent endometriosis is possible. Studies suggest that endometrial tissue can regrow within a few years after surgery, particularly if hormonal therapy isn’t used as a follow-up treatment.
What are the pregnancy chances with stage 4 endometriosis?
Stage 4 endometriosis significantly reduces natural conception chances due to scarring, adhesions, and ovarian cysts. However, assisted reproductive techniques like IVF can still offer a path to pregnancy for many women.
How is stage 4 endometriosis diagnosed?
Diagnosis typically involves a pelvic exam, ultrasound, MRI, and confirmation through laparoscopic surgery. A laparoscopy is currently the gold standard for staging endometriosis accurately.

Daniel Morgan is a health writer and wellness researcher dedicated to making evidence-based health information simple, practical, and actionable. With over six in health education and research, he specializes in translating complex medical topics into clear guidance readers can trust.